 
Remember that if you can’t see in, the patient can’t see out. Is there something blocking the view (media opacity)? Many ocular disorders- corneal disorders, anterior uveitis or hyphema, cataracts, and vitreous inflammation or hemorrhage-decrease the normal transparency of the ocular media, thereby obstructing the view of the fundus ( ▶ Fig. Is the pupil too small? (Did you forget to dilate the patient’s pupils?)Īre you sure you know how to use the ophthalmoscope? Is the ophthalmoscope working? (are the batteries charged?) If you are unable to see the fundus on examination, review the following checklist: Besides the smaller and thinner caliberappearing as fine tufts or frondsretinal neovascularization is often accompanied by connective or fibrotic tissues that increase in intensity over time. Got normal colour vision on this test, but the original image still took. Nearly all patients who say they have glaucoma have open angle glaucoma, which does not contraindicate pupillary dilation. The characteristic of different retinal features such as blood vessels, blood capillaries, OD, macula and fovea change due to different pathological conditions. To identify retinal neovascularization, key features on fundus exam help distinguish it from normal retinal vasculature. Color vision is possible due to photoreceptors in the retina of the eye known. Patients who know they have a diagnosis of angle closure glaucoma will already have been treated with laser to prevent episodes of angle closure from pupillary dilation and can therefore be dilated without risk. Glaucoma is not a contraindication for pupillary dilation. Do not dilate a neurosurgical or unstable patient, because monitoring of the pupils may be important. 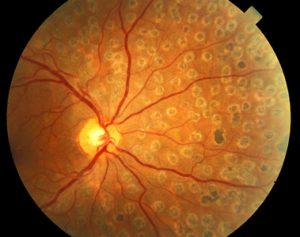
Always document the time of dilation and the drops used. It is always better to dilate both eyes rather than one eye (a unilateral mydriasis is often alarming, whereas most people will not be concerned about bilateral mydriasis if the patient is awake and alert). Use the 20-D lens to evaluate macular and peripheral pathology. 20 D: The most commonly used binocular indirect ophthalmoscopy (BIO) lens, the 20-D double aspheric lens has magnification up to 3.13° and a 60° dynamic field of view. Young patients will have difficulty reading after pharmacologic dilation because of the blockage of accommodation. You have two main options for indirect ophthalmoscopy. Long-acting dilating drops (used as cycloplegics), such as cyclopentolate, homatropine, and atropine, should not be used to view the fundus (the dilation and cycloplegia may last from 12 hours to up to 14 days).īe sure to alert the patient that driving may be difficult after dilation, especially in bright sunlight. It permits to define the location and nature of the changes in the retina and adjacent structures and objectively evaluates the thickness of the retina and. Dilation occurs within 30 minutes and usually resolves within 6 hours. To dilate the pupils use a combination of short-acting agents that block parasympathetic transmission (tropicamide) and enhance sympathetic activity (phenylephrine). 
To view the ocular fundus to the best advantage, the pupils should be dilated. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
